Sensory overload
Rare testing of the stomach at Mayo Clinic
Ice cream is a huge motivator for me (even though my body hates dairy). I will drive a distance for it, create reward systems based on it, and wait in line for just the right consistency and flavor. I think that espresso mixed with ice cream is one of the tastiest concoctions on the planet and the right ice cream is worth notable abdominal discomfort.
And so, it is with ice cream that I mentally channeled myself through the experience of a small bowel manometry at Mayo Clinic six weeks ago. This procedure, which investigates motility dysfunction, is not performed anywhere else in the country and is only conducted at Mayo 4-6 times a year!
Promising myself that I would get a big dish of Flapdoodles ice cream after the procedure, I started with the dreaded seven hours without water – always a significant hurdle of procedures / surgeries. (IYKSYK – If you know Sjogren’s, you know.) My mouth gets so dry that saying no liquids whatsoever after midnight feels impossible. I limp by with putting water in my mouth and spitting it back out.
The preliminary obstacle, though, was not that, or knowing that I’d miss both Ian’s first piano recital and Cali’s choir concert to take this appointment – the next procedure availability would not be until November. (Missing important moments with my kids is what I grieve most.)
It was not the drive to the Cities – literally threading the needle through storms – to meet up with my friend Meghan, the so-so overnight in a cheap hotel, or the IV insertion, which usually requires hot towels and an ultrasound. Instead, it was figuring out how to stabilize a tube down my throat without touching my lower teeth and gums.
As they prepped me in the procedure room for an upper endoscopy, the presiding doctor reminded me that they wouldn’t be able to put me to sleep, since I needed to be fully awake for testing. I tried to be easy-going and humorous, saying out loud, “If I can give birth without pain meds, I can do this.” He responded, “Well, that’s more than I can do.”
Getting serious, I shared my first fear – that the bite clock would trigger nerve pain in a new tooth and I’d again encounter intractable rising pain, leading to a desperate plea for extraction.
I asked for a pediatric bite block to avoid jaw pain but, with five missing lower front teeth, the block was too small to land on any lower molars. So, we went with the average adult block, which my back molars could grip. I was very nervous, because I’d have to bite down hard on it for a long period of time. I cared too much for answers, though, to pull the plug on the whole thing.
They popped in the bite block, taped it in place, turned me on my left side and I blessedly don’t remember the rest of the upper GI procedure. Thanks Versed.
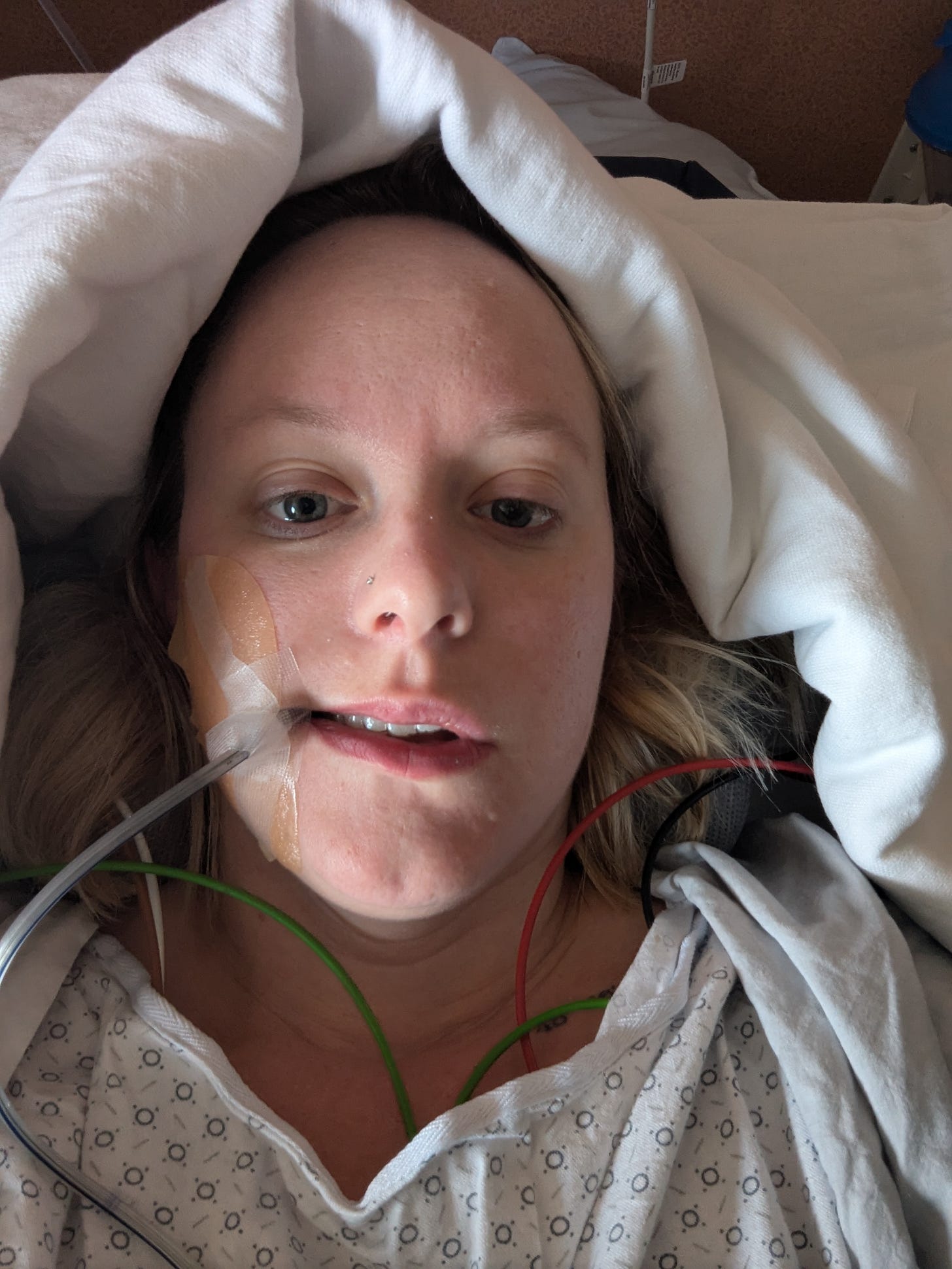
I woke up in a hospital bed with a tube down my throat (through my stomach into my upper small intestine), taped to the side of my upper right teeth. For the next 5ish hours, every single swallow was very painful. (Do you know how many times you swallow in five hours? – 300, that’s how many.)
I had a neck pillow and my own blanket with me – not my first rodeo, hospital blankets are like heated paper. Despite these self-accommodations, neck and occipital pain rose from lying on my back without moving.
During a small bowel manometry, or antroduodenal manometry, the medical team evaluates the muscle contractions of the stomach and small intestine to assess the strength and coordination of these functions. A catheter with sensors records pressure changes caused by the contractions, and they get a sense of any motility abnormalities.
Partway through the testing, I had to eat ground chicken, buttery mashed potatoes and pudding. Thankfully, I could mix them together to get the chicken down but my brain thought the tube was food, too, so would convulsively try to swallow and clear my throat after each bite. You are timed for this lunch and have to eat as much of it as you can.
Around this point, the pain in my throat and in the back of my head and neck was so extreme that I begged for medication. Anything that would slow my digestive processes, like opioids, were not an option but they consented to give me Toradol via IV, which helped tremendously, as did having Meghan beside me.
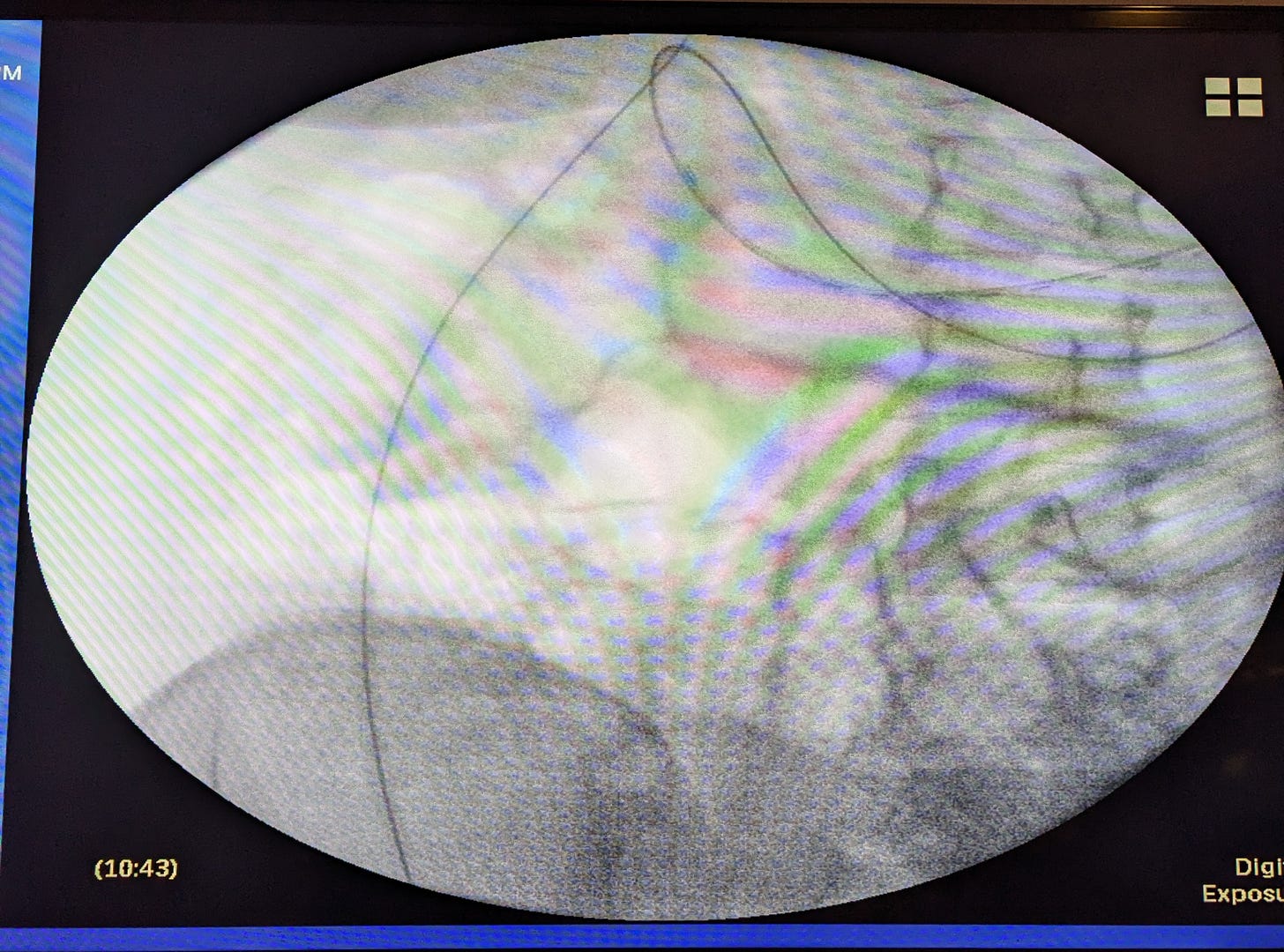
Somewhere into the third or fourth hour, they wheeled me back to the procedure room and placed me under the fluoroscopy so a second doctor could check the placement of the tube. As he gave cues, a nurse pulled the tube out a little, giving me a nice taste of bile. I was like a weird magic trick in which an endless amount of scarf is pulled from a hat.
Back in the testing room, I almost made it the full, expected six hours, but with about a half hour left to monitor, I had to pee so badly that my pelvis and abdomen throbbed.
I don’t know if you’ve ever had a bed pan, but it’s exactly what it sounds like. We pulled my underwear down, put a pan underneath me and I tried to let loose. And, wow, is that hard to do! My brain simply wouldn’t do it. I couldn’t pee, even when the nurses gave me privacy and I sat up. They told me this was common.
I made it perhaps twenty minutes further after attempting to empty my bladder and then my brain screamed that it could go no further. I told the nurses that a migraine was building and that if we didn’t pull the tube now, they’d have to transfer me straight from GI to the emergency room for a migraine cocktail.
I was afraid that all I had endured would be for nothing, that they didn’t have enough data, but the nurse said, “Actually, most people don’t make it the full six hours and a lot of people aren’t able to even get the tube placed.” Oh, that would have been helpful to know for encouragement!
They removed the tube – way easier out than in. I rinsed puke from my mouth, we removed all the sensors, I shuffled to a toilet, and I was free to leave.
We went to draw blood at the Lab and maneuvered our way to the parking ramp. At that point, I knew ice cream was a no go. As a migraine obliterated any thought but survival, we drove past Flapdoodles.
Meghan transported me back to the St. Paul in pouring rain while I lay curled in fetal position in the passenger seat, holding my head and a puke bag, covering my eyes. When we got to Meghan and Ryan’s house an hour and a half later, they helped me to my guest room and I called out essentials – “get me a puke bucket, ice cap, white noise, Zofran, Imitrex, muscle relaxant” – and I passed out. Thankfully the pain went down after a few hours and I was able to get up, eat and talk with my friends.
The next morning, Meghan and I walked around her beautiful neighborhood and I packed and left for home.
The results?
I had a video call with the leading physician a week later. I was grateful to learn that they believe my small intestine functions normally. (I was really surprised because Sanford Health in Fargo had told me I needed my colon removed!) The muscles around the lower part of my stomach, however, do not grind up food like they should. There is poor coordination between the nerves there and the muscle contractions they dictate.
What this means?
I keep doing all physical therapy and taking all the meds and supplements I have been. Continue to take small bites, chewing thoroughly, and eat softer foods, considering a liquid diet when the pressure in my upper abdomen is extreme. And, I return to Mayo in August for an autonomic reflex screen, sweat test and lab work to investigate an autonomic nervous system dysfunction.
I am also on a wait list to see a Mayo rheumatologist and neurologist. Coordinating these all into one visit is probably not possible but I get calls or texts almost every day proposing dates and times.
So that’s that. While I await further exploration, I’m mitigating usual mouth pain and new pain in my forearms, wrists and hands, which will have to be another story.
In the now, I need to have a little ice cream.





Love you girl. You were a warrior thought that day!! I was so glad to be there with you.